 The majority of patients are asymptomatic at presentation or have mild blurred vision. The typical patient presents for an ophthalmologic exam and incidentally is found to have PPRCA. Late in the disease, the RPE is affected and is associated with areas of reduced choroidal thickness. In early stages of the disease, the outer retinal layers are thinned (including outer nuclear layer and external limiting membrane) and the choroidal thickness is reduced, while the RPE is not affected. The use of spectral-domain optical coherence tomography (SD-OCT) combined with fundus autofluorescence allows for in vivo characterization of the disease. No known histopathological examinations have been completed on a human eye. The RPE layer was partially disrupted with Bruch’s membrane intact. The inner plexiform layer and ganglion cell layer were reduced. The retinal atrophy was characterized by loss of photoreceptor outer segments, outer nuclear layer, and inner nuclear layer. On histopathological examination the areas retinal atrophy transitioned to normal retina abruptly. In a study by Linek et al, five dogs with funduscopic changes similar to human findings of PPRCA were observed and a histopathological examination was completed for one case. PPRCA involves both the RPE and the choroid. PPRCA is characterized by retinal pigment epithelium degeneration, choriocapillaris atrophy and pigmentation along the retinal veins. There have been a few cases of familial occurrence, but currently no known genes have been identified with the disease. The disease is more common in males than females in the reported literature here. However, no known systemic diseases have been identified as the cause of the retinal findings. Many inflammatory and infectious causes have been associated with the disease, including sarcoidosis, Behcet’s disease, syphilis, measles, rubeola, and tuberculosis. The etiology of PPRCA remains unknown with a presumed initial inflammatory insult that leads to the slow developmental of the retinal findings. The general accepted name of the disease is either paravenous chorioretinal atrophy or pigmented paravenous retinochoroidal atrophy. Since then, it has appeared in the literature under multiple names including retinochoroiditis radiata, pseudoretinitis pigmentosa following measles, chorioeeretinitis striata, congenital pigmentation of the retina, melanosis of the retina, paravenous retinal degeneration, pigmented paravenous chorioretinal degeneration, pigmented paravenous chorioretinal atrophy and PPRCA. 
He termed the disease retino-choroiditis radiata. Hewitson-Brown associated the retinal findings with tuberculosis. 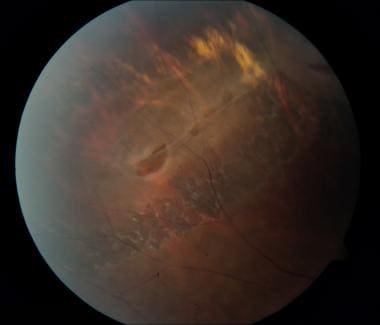
Given the patient’s exposure to tuberculosis, Dr. An ophthalmic examination was remarkable for bilateral pigmentary changes along the distribution of retinal vein (Figure 1). The initial case was a 47 year old male with past exposure of tuberculosis (multiple family members) was admitted for alopecia areata. The disease was first described in 1937 by Hewitson-Brown. The diagnosis is made with a clinical examination due to the peculiar retinal findings. Pigmented paravenous retinochoroidal atrophy (PPRCA) is a rare disorder of unknown etiology and the natural course is poorly understood. The findings are usually incidental with minimal effect on vision. The disease is characterized by pigment accumulation along the distribution of retinal veins. Pigmented paravenous retinochoroidal atrophy (PPRCA) is a rare disorder of unknown etiology. Figure 1: drawing of the first reported case PPRCA by Hewitson-Brown, which he termed retino-choroiditis radiata. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
